 About 90% of patients with atrial flutter electrically converted can be discharged with low incidence of stroke in one year 2.Consider cardiology consult prior to discharge.Longer duration of symptoms prior to ED presentation.On-going medical management (pulmonary edema, myocardial ischemia, respiratory distress).If thrombus identified, defer cardioversion.Must be pretreated with heparin and continue with OAC for four weeks.If no thrombus identified, can proceed with cardioversion.If timeframe unknown or high risk of stroke, can perform transesophageal echocardiography to evaluate for left atrial thrombus.If Rate does increase with increasing CHA 2DS 2-VASc score (0.4% with a score of 0 versus 2.3% in those with a score of 5 or greater) 11.Thromboembolic event rate without anticoagulation in this cohort of patients is around 0.7% 11.Cardiovert without anticoagulation if there is a very clear history that onset of flutter was Thromboemboli is due to existing thrombi within the atrium at the time of conversion or the formation of one after conversion in the setting of depressed atrial function.No difference in risk of thromboembolic event between pharmacologic versus electrical cardioversion 11.Use a scoring system such as CHADS, CHA 2DS 2-VASc for evaluation and determination of risk of thromboembolic event.Due to risk of torsades, it is contraindicated in patients with hypokalemia, prolonged QT, or heart failure.Infusion: 5 mg/h, titrate by 5 mg/h to max of 15 mg/h (to 20% reduction in HR or HR 60 kg- 1 mg IV over 10 min 4.Second (if no reduction in HR by 20% or HR >100 bpm): 0.35 mg/kg (15-25 mg) IV 9.Initial: 0.25 mg/kg (10-20 mg) IV bolus over 2 minutes.Diltiazem: increases refractory of AV node → slows conduction through AV node → decreases ventricular rate.Since the rate is determined by the AV node, drugs that slow AV conduction are used.Indications: immediate rate control to reduce symptoms in stable patient or chronic therapy to prevent symptoms or cardiomyopathy 9.Adenosine can transiently block the AV node to reveal flutter waves and can help diagnose.Flutter has at least as high of a risk for thromboembolic event as AFib → same risk stratification for anticoagulation as in AFib 7.Chronic flutter with RVR can lead to tachycardia-induced cardiomyopathy 4.A rapid ventricular rate decreases the ventricular filling time and, this coupled with asynchronous atrial to ventricular contraction, can lead to heart failure 2.Dyspnea, angina, or palpitations, and less likely hypotension or syncope.Symptoms are largely dependent on the ventricular rate.Flutter can either be paroxysmal or persistent, and patients can either be asymptomatic or symptomatic.Patients can develop atypical atrial flutter after AFib ablation due to circuits created by scarring.Can occur after starting an antiarrhythmic drug for AFib.Similar risk factors for AFib: pulmonary disease, diabetes, HTN, older age, obesity, and thyrotoxicosis 5.Uncommon to occur in a structurally normal heart or without a predisposing event or preexisting comorbidity.Incidence in the US is 200,000 new cases per year 5.80% of patients with atrial flutter are male 6.ECG will be different than typical/reverse flutter.Typically associated with structural heart disease, cardiac surgery, or ablation 5.Atrial tachycardias that are caused by a reentrant circuit that do not involve the cavotricuspid isthmus but any portion of the atria 5.Positive flutter waves in inferior leads and negative atrial deflections in V1. 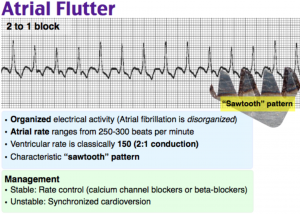
If re-entry is clockwise, this is “reverse” typical flutter.Negative flutter waves in inferior leads II, III, aVF and positive atrial deflections in V1 4.Circuit typically rotates in a counterclockwise direction → “sawtooth” EKG pattern. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
